
Walk into any grocery store, and you’ll see aisles filled with colorful bottles promising everything from “immune support” to “brain power.” In the United States alone, people spend billions of dollars a year on vitamins and supplements.
However, scientific research shows that for most healthy people eating a regular diet, these pills offer little to no benefit. So, why do we keep taking them, and when do they actually become dangerous?
By the way, I’m a 40+ year licensed physician who has studied supplements for the past 16 years.
The Psychology of “Just in Case”
If science says they don’t help, why is the industry booming? There are a few psychological reasons:
The “Insurance Policy” Mentality: Many people take a daily multivitamin as a safety net. They think, “Even if it doesn’t help, it can’t hurt.”
The Appeal of Naturalism: We often fall for the “appeal to nature” fallacy — the idea that because a supplement comes from a plant or a mineral, it is automatically safer than a “synthetic” medicine.
The Illusion of Control: In a world where we can’t control pollution or aging, taking a pill feels like an active step toward “doing something” for our health.
When Supplements Become a Waste of Money
For the vast majority of people, a multivitamin is essentially “expensive urine.” Your body is highly efficient; it takes the vitamins it needs from your food and flushes the excess out through your kidneys.
If you eat a diet that includes fruits, vegetables, proteins, and grains, you are likely already hitting your targets. Taking a multivitamin on top of that doesn’t make you “extra healthy” — it just gives your kidneys more work to do. Furthermore, some studies have shown that long-term use of multivitamins doesn’t actually lower the risk of heart disease or cancer.
The Hidden Dangers: When “Natural” Hurts
The “it can’t hurt” mindset is actually a dangerous myth. Because supplements are not regulated as strictly as prescription drugs, they can have side effects or even toxic levels of certain nutrients.
Vitamin A (Beta-Carotene): While Vitamin A is good for your eyes, taking too much in supplement form has been linked to an increased risk of lung cancer in smokers and can cause liver damage.
Vitamin E: High doses of Vitamin E supplements have been associated with an increased risk of heart failure and even premature death in some clinical trials.
Calcium: Getting calcium from cheese and kale is great for bones, but taking high-dose calcium pills has been linked to a higher risk of calcium buildup in the arteries (plaque), which can lead to heart attacks.
The Bottom Line
There are absolutely cases where supplements are necessary — such as Vitamin D for people in northern climates, B12 for vegans, or Folic Acid for pregnant women. However, these are specific medical needs.
Taking a handful of pills without a blood test to prove a deficiency is like adding extra oil to a car that is already full; it doesn’t make the car run better, and it might just gunk up the engine.
Nutrient Comparison: Food vs. Pills
Here is how easily a “regular diet” outpaces a supplement. Most people don’t realize that the vitamins in food are often absorbed better by the body because they come with fiber and healthy fats.
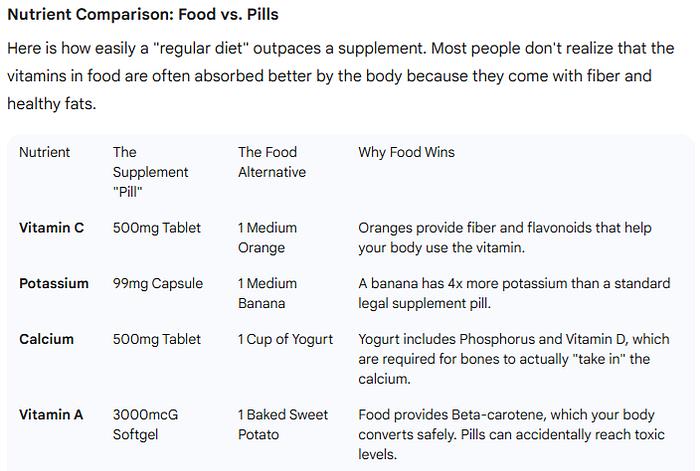
Some food versus pill comparisons
The “Waste” Factor: Absorption vs. Elimination
When you swallow a pill that your body doesn’t need, it follows a specific path. Because your blood is already “saturated” (full) with vitamins from your breakfast or lunch, your liver and kidneys have to work overtime to filter the supplement out. That’s not a good thing.
Also, since supplements are not prescribed, no one does a contraindication check with your existing medications and that can be disastrous.
For example, CoQ10 often recommended for people taking statins, can also interfere with the ability of blood thinners to do their job, which is to prevent blood clots from forming. Probiotics taken within two hours of taking an antibiotic can reduce the effectiveness of the antibiotic medication. There’s evidence that ashwagandha, increasing in popularity, can interact with drugs used for diabetes and high blood pressure, as well as immunosuppressants, sedatives, anti-seizure medications and thyroid hormone medicines. Consulting a physician is always smart when combining prescribed medications and supplements.
Why We Still Take Them
The supplement industry spends millions on marketing to make you feel “incomplete.” They use terms like “Bio-available” or “Clinical Strength” to sound scientific. In reality, the most “clinically proven” way to stay healthy is a varied diet and early disease detection, not a bottle of pills.
So if you want to keep supplement makers fat and happy, keep spending your hard earned money indiscriminately based on their effective marketing.
Important Note: Never stop taking a supplement that was specifically prescribed by your doctor for a diagnosed condition (like anemia or osteoporosis) without consulting a physician.
HSA/FSA Eligible
Doctors Are Human.
That's Why There's Medome.
Start your free trial today. No credit card required.
Start Your Free Trial
Join thousands protecting their health with AI that never forgets

Critical details get missed when your health information is scattered. Medome connects the dots across your complete record.
Start Your Free Trial
Get In Touch
Email: service@medome.ai
Phone: (617) 319-6434
This is Dr. Steven Charlap's cell. Please text him first, explaining who you are and how he can help you. Use WhatsApp outside the US.
Hours: Mon-Fri 9:00AM - 9:00PM ET